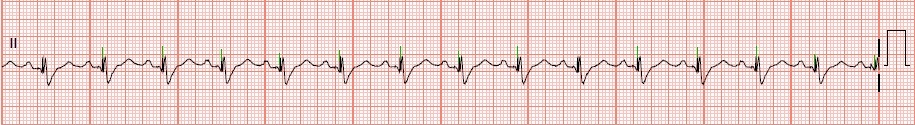
Others may have a mechanical tricuspid valve, which prevents passing the LP into the right ventricle. 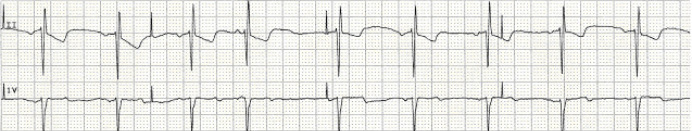
They may require the more complex features and programmable technologies available in dual-chamber and biventricular pacemakers. Some patients aren’t good candidates for an LP. (Note: For pacing code information, visit /?p=52458.) Patients with existing pacemakers who’ve had surgical pocket or trans – venous lead complications also may benefit from this technology. Patients who require a VVIR (ventricle pacing, ventricle sensing, paced beat inhibition, rate modulation) for symptomatic bradycardia may be candidates for the LP. Micra’s battery life is expected to be 10 years or more. Crotti reports that Abbott is now planning to focus on developing the dual-chamber leadless pacemaker, as this is where the greater need is. No other adverse outcomes have been reported. To date, 34 patients have experienced battery depletion with the Nanostim. The manufacturer recommends device replacement for anyone with the Nanostim LP starting with those who’ve had the pacemaker for the longest duration. Jude Medical (now Abbott) conducted clinical trials of its Nanostim LP, but after 1,423 implants, the company halted implantation in October 2016 because of seven reports of battery issues that resulted in lost telemetry and pacing output. As of October 2017, Medtronic reports that more than 10,000 patients in 40 countries have a Micra LP.Ĭurrently, Micra LP is the only LP on the market. Vascular closure of the femoral vein, using manual pressure, purse-string suture, or a vascular closure device, prevents bleeding at the groin site. After it’s fixed to the inside of the right ventricle, the catheter and introducer are removed. It’s inserted with a catheter through the femoral vein with a 23 French introducer, advanced into the right ventricle, then attached to the endocardium. (See Pacemaker comparison.) The device is 25.9 mm long, 6.7 mm wide, and weighs 2 grams. Medtronic won Food and Drug Administration (FDA) approval to market the Micra LP on April 6, 2016. 
In the United States, just 20% of patients who required permanent pacemakers received traditional single-chamber devices, while the remaining 80% received traditional dual-chamber devices. The 2009 world survey by Mond and Proclemer provides prevalence data on the use of pacemakers by type. LPs are single-chamber devices, so currently they’re available only for a limited number of pacemaker candidates. LPs, which are miniature devices, are implanted directly into the right ventricle via the femoral vein in the groin. The LP was developed to avoid the complications associated with the leads and surgical pocket required when placing a traditional pacemaker. Understanding this new technology will help you deliver safe care to patients who may be candidates for an LP or who may already have one. Many nurses may not have encountered a patient with an LP and little nursing literature on the topic exists. (See Traditional pacemaker basics.) However, as with any new technology, a knowledge gap exists. This device is one of the biggest advancements in pacemakers since they came into use for symptomatic bradycardia more than 50 years ago. ONE of the most recent developments in cardiac pacing is the leadless pacemaker (LP). Currently, leadless pacemakers can pace only from the right ventricle.The leadless pacemaker eliminates the complications of conventional pacemakers related to leads and surgical pocket complications.The leadless pacemaker is a right ventricular single chamber pacemaker used to treat symptomatic bradycardia.Learn about the nursing implications of these innovative devices. Author Guidelines and Manuscript Submission.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
